Hidradenitis Suppurativa, known as HS for short, is a skin condition which not that many people have heard of, but it’s worth knowing about. Because it has a lengthy name (which is difficult to spell and pronounce!), that could create the impression it’s an obscure issue, particularly compared to well-known skin conditions which have short and memorable names, like acne and hives.
But Hidradenitis Suppurativa is more common than you probably think. You could even have it right now without even realising it since it can be mistaken for other illnesses. HS is far less common than conditions like acne, but it is a lifelong, recurring condition that can have distressing effects if not treated properly. Organisations including the NHS report that HS is estimated to affect about 1% of the UK population, meaning it’s common enough to affect millions of people.
Because of how serious the condition is, an annual and global awareness week for the condition has been established and it is currently taking place this week. So here’s a summary of what’s worth knowing about this condition, including how exactly it affects people, how it can be identified and how best to treat it if you have it.
What exactly is Hidradenitis Suppurativa?
Hidradenitis Suppurativa is a condition that creates abscesses (collections of pus) and scarring on the skin and causes mild to severe pain. HS can cause all sorts of different lumps to appear on the skin including cysts, blackheads, scarring and red boil-like lumps. These lumps can leak both pus and blood.
HS affects areas of the skin which contain apocrine sweat glands. These glands are found mostly in the armpits, breasts, buttocks and groin. As a result, the problem can also develop on the genitals and around the anus (back passage). In some cases, abscesses have spread to the nape of the neck, the waistband and inner thighs.
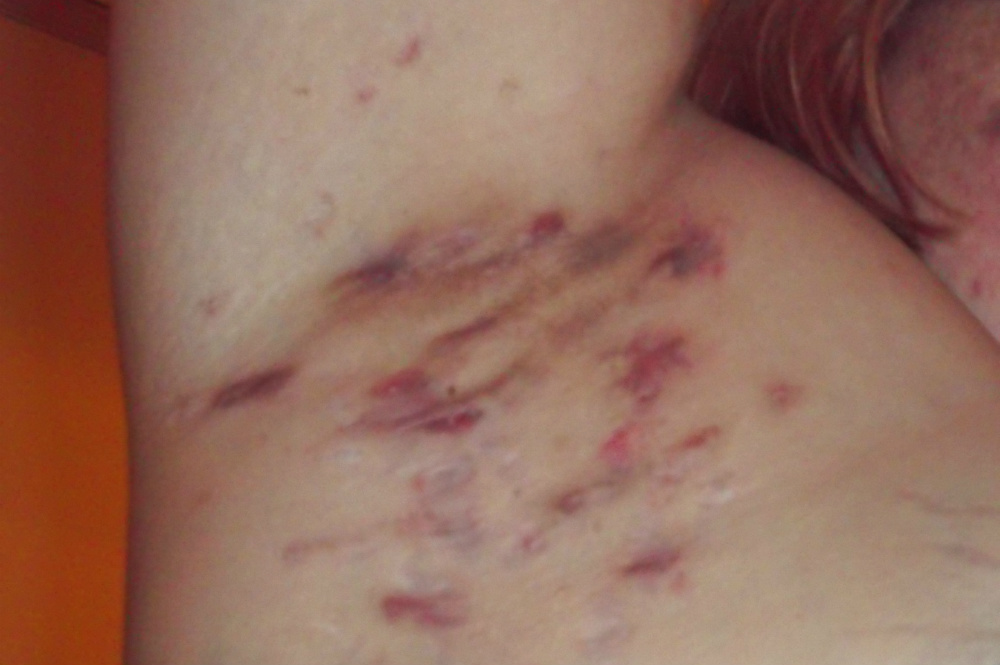
Credit: BRI72783
Often the condition will start with a small and firm lesion in one area of the body. This will eventually disappear or rupture (releasing pus), but the amount of time this takes after it first appears can range between a few hours and a few days. New lumps will then appear in another area of the body near where the first lesion appeared.
Some of the lumps can become infected with bacteria, creating a secondary infection which will require antibiotics to treat.
How do you diagnose Hidradenitis Suppurativa?
The lumps associated with HS are a result of blocked hair follicles. Such an issue can also cause conditions such as acne and ingrown hairs. However, whereas a clear reason can be given for other skin conditions, the exact cause of Hidradenitis Suppurativa is not certain.
What prevents diagnosing this condition from being straightforward is that its symptoms resemble other conditions, so misdiagnosis on multiple occasions is possible. For instance, if the symptoms occur around the groin or backside, it could initially be assumed that the cause is a sexually transmitted disease (STD).
There is no test which specialises in identifying HS. However, a doctor can make an accurate diagnosis by examining the symptoms, the areas of the body they’re occurring on and by factoring in a patient’s history.
What could cause Hidradenitis Suppurativa?
Popular theories on how someone can develop HS relate to potential imbalances in a patient’s hormones.
It is theorised that hormones may be involved in the control of apocrine sweat glands, so an imbalance in hormones could disrupt how these glands work and cause HS. Adding weight to this theory is the fact that HS usually starts around puberty (although not in all cases). The condition is also more often reported among women than men, and it has been found it can get worse for women during menstrual periods (controlled by hormones).
Hormone-related conditions which HS has been frequently linked to include acne and hirsutism (excessive hair growth). Another is Polycystic Ovary Syndrome (PCOS), which affects how the ovaries work. Intriguingly, PCOS often runs in families and HS could have the potential to become a hereditary condition too. Sources including the British Skin Foundation have found that Hidradenitis Suppurativa runs in the families of about one-third of those with the condition.
Another theory on HS is that it can occur when bacteria which normally lives on the skin becomes trapped in blocked glands or hair follicles. However, not that many cases of HS feature a bacterial infection as a symptom, and when it does occur it’s usually a secondary condition.
While HS can occur for non-smokers of normal weight, it’s believed that smoking and being overweight can aggravate the condition considerably. It has been confirmed that poor hygiene does not directly cause HS, but maintaining good standards in this area is a good idea nevertheless!
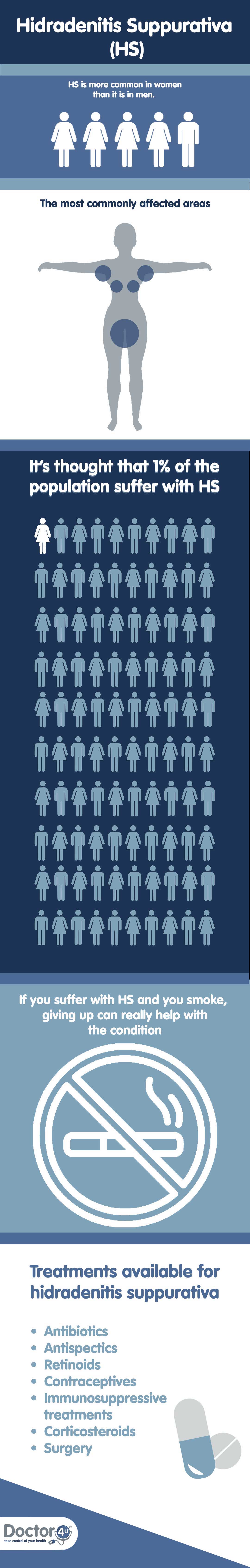
Can Hidradenitis Suppurativa be cured?
Unfortunately, there is no cure for Hidradenitis Suppurativa and it typically persists for many years. But while there’s no way of switching it off, it can become inactive when the right treatment is involved. Another positive thing is that HS is not contagious, so it cannot be passed on to someone else by contact.
How do I treat Hidradenitis Suppurativa?
Treatment for Hidradenitis Suppurativa is tuned to fit individual patients and depends mainly on the severity of the condition. The earlier this condition is diagnosed, the easier it should be to manage it.
Earlier, less severe strains of this condition can be controlled with medication. If you have lumps which are really painful, inflamed or oozing pus, then you may be prescribed a one or two-week course of antibiotic tablets to deal with any potential bacterial infection. If such an infection is not present though, then low-dose antibiotics (probably tetracycline) could be taken for at least three months. Other antibiotics including erythromycin, lymecycline and doxycycline may also be utilised.
Antiseptic lotions and washes are also frequently prescribed to patients, with 4% chlorhexidine wash and clindamycin being popular examples. If a female patient has flare-ups of HS before each of their periods, then they may benefit from taking a combined contraceptive pill. Retinoids, which include vitamin A-derived tablets like isotretinoin and acitretin, may also help but should be used with caution and avoided by pregnant women.
When wanting to drain lumps filled with pus, a warm flannel applied to the affected skin or taking a bath can suffice. Painkillers including non-steroidal anti-inflammatories may be prescribed to ease the feelings of pain and inflammation caused by HS.
In more severe cases where persistent discharge or inflammation is occurring even with medical treatment, surgical treatment may be required. This may involve removing small areas where repeated inflammation is occurring, or wider procedures that take away all the affected tissue. Wider procedures reduce the chance of HS returning in the treated area compared to smaller procedures, but healing times are usually longer. In the most severe cases of HS, patients may be given immunosuppressive treatments by injection if other treatments prove ineffective.
Non-medicinal help
In terms of how your lifestyle can help deal with HS, we mentioned before that avoiding smoking and losing any excess weight can make a big positive difference. On top of that, washing with antiseptic soaps or bath additives, avoiding tight clothing and using stress management are all recommended as well. Some patients have reported flare-ups of HS after wearing tight clothes or while going through stressful periods in their life.
Even with treatment, living with HS can be a big challenge for the mind. Not only does managing the condition influence your daily routine, but the symptoms can also create a lot of pain, discomfort and embarrassment. This can strongly impact on your quality of life and state of mind, so it’s worth considering support charities as well as the various treatments already mentioned. There are some support groups which are specifically dedicated to helping people who have HS, with The Hidradenitis Suppurativa Trust being a prime example.