HIV Statistics UK
In January this year, the UK’s Health Secretary, Matt Hancock, pledged to end HIV transmission by 2030, meaning that the country has 11 years to bring the rate of new diagnoses down to zero, but how close to this figure are we all ready?
Data from HIV Prevention England states that during 2017, there were 4,393 new diagnoses of HIV, which is a considerable reduction on previous years. In fact, from 2007 to 2017, the UK saw a 41% decrease in new HIV diagnoses, which equates to almost 3,000 fewer people.
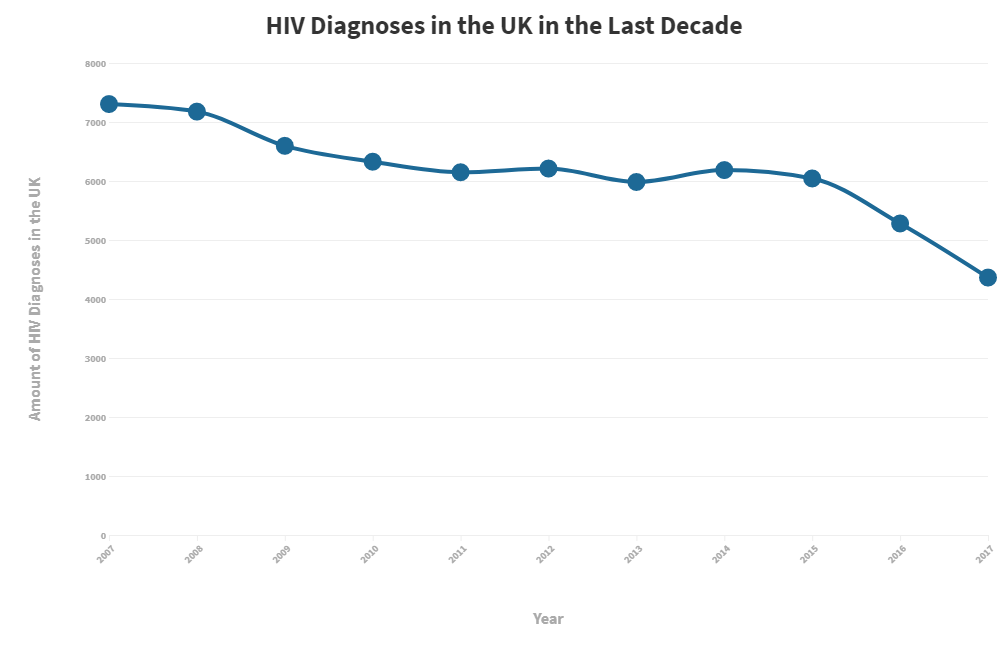
So how likely is it that UK HIV rates will be at zero in 2030? Overall, HIV statistics for the UK show that the trend for new diagnoses has been declining steadily over the last decade, with the most progress being made from 2015-2017. However, the average decrease in new diagnoses per year is only 5.1%, so if this continues to be the case, the government’s targets may not be met. For HIV to be eradicated in the UK by 2030, more support needs to be put into place for those that need it, and figures will need to decline by at least 40% per year between now and 2030 – eight times the current rate.
However, seeing a significant decline in 2016 & 2017 (13% & 18% respectively) gives us hope that prevention methods such as condoms and PrEP are working well. As long as the government supports those at risk of HIV by making PrEP accessible, a 0% rate of transmission could be possible by 2030.
What is HIV?
HIV stands for human immunodeficiency virus. According to the NHS, HIV is a condition that can cause damage to the cells in your immune system, which weakens its ability to fight everyday infections and diseases. Someone with HIV is said to be HIV-positive, whilst someone without it would be HIV-negative.
If HIV stays untreated, it can severely damage the immune system, causing a much more serious condition known as AIDS (acquired immune deficiency syndrome) that can carry potentially life-threatening complications. Although HIV can’t be cured, there are treatments available to manage the condition by lowering the viral load in the body and in many cases, these treatments consisting of antiretroviral drugs can cause an HIV-positive person to become undetectable. Being undetectable doesn’t mean that HIV has vanished, but it does mean that it’s unable to be passed on due to the viral load being so low.
HIV is transmitted through bodily fluids such as
- Blood
- Semen
- Pre-seminal fluid (pre-cum)
- Vaginal fluid
- Anal mucus
- Breast milk
The virus can only be transmitted by someone that has a detectable viral load, and the most common ways of transmission include unprotected sex, sharing drug injecting equipment or sex toys, and by coming into contact with HIV-positive blood (especially if the blood touches one of your body’s mucous membranes). Mothers can also transmit the virus to their children.
HIV is known to affect certain demographics more than others, for example, groups that have been statistically proven to be at higher risk of acquiring HIV include:
- Men and trans women that have sex with men (MSM)
- People of black African origin
- Those who share drug injecting equipment such as needles or syringes.
Luckily, with medical advances, HIV is now a preventable condition with medicine often known as PrEP. PrEP stands for pre-exposure prophylaxis and can help to stop the virus from taking hold in your cells, proving to be 99% effective in some cases.
How Common is HIV in the UK?
According to Avert UK, HIV statistics in the UK estimate that 102,000 people are living with HIV. Given the population, this means that roughly 0.16% live with the condition, and a vast majority (98%) of those affected are on treatment to control the virus. As we saw earlier, HIV rates in the UK are declining, and these are set to fall even further as clinical trials are taking place to determine the demand for PrEP. Unfortunately, the drug isn't yet available on the NHS in England unless you're part of the IMPACT trial, but with places being difficult to get hold of, many of those in need are having to pay for a private prescription.
Each year in England, the government publish an “Annual Epidemiological Spotlight on HIV” for each of the 9 regions in the country, broken down by upper-tier local authorities (UTLA). Our team has compiled the most recent data (2017) to provide an insight into HIV in England.
Part of the data included in the government publications included the average amount of new HIV diagnoses per 100,000 people in each UTLA. We then found the population for each of these areas and were able to calculate an estimate of actual HIV diagnoses based on the annual spotlight papers. With these figures, we could then filter the results by the highest number of new HIV diagnoses, as well as the density of new diagnoses per region and per UTLA.
Unfortunately, equivalent data wasn't available for Scotland, Wales and Northern Ireland
HIV in England
To obtain results for each region, the population of each UTLA in a region were totalled, as well as the number of new diagnoses of HIV (based on the figure per 100,000 people). The figures showed HIV statistics for each of the 9 regions in England. These were then able to be ordered by the volume of new diagnoses per region, and the results are as follows:
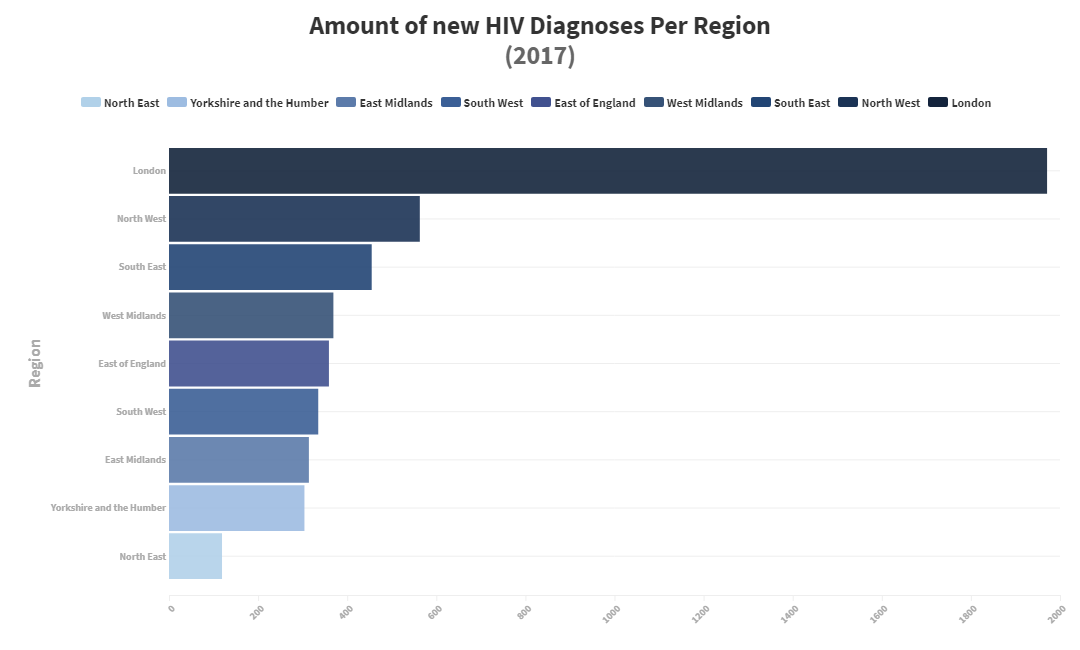
From the graph, it’s clear to see that London had the most instances of HIV diagnoses in 2017 by a mile, with a whopping 72% more than the North West, whilst the North East has noticeably fewer than anywhere else. In fact, it has 61% fewer HIV diagnoses than Yorkshire and the Humber, which is only one place above it. This means that there is a 91% difference between London and the North East, but there's an explanation for the huge differences. When looking at the results, we also included the population of each area in the data and found that there was a positive correlation between regional population and HIV in England. For example, in areas where the population is higher than average, HIV diagnoses were also increased. The graph below should explain the trend.
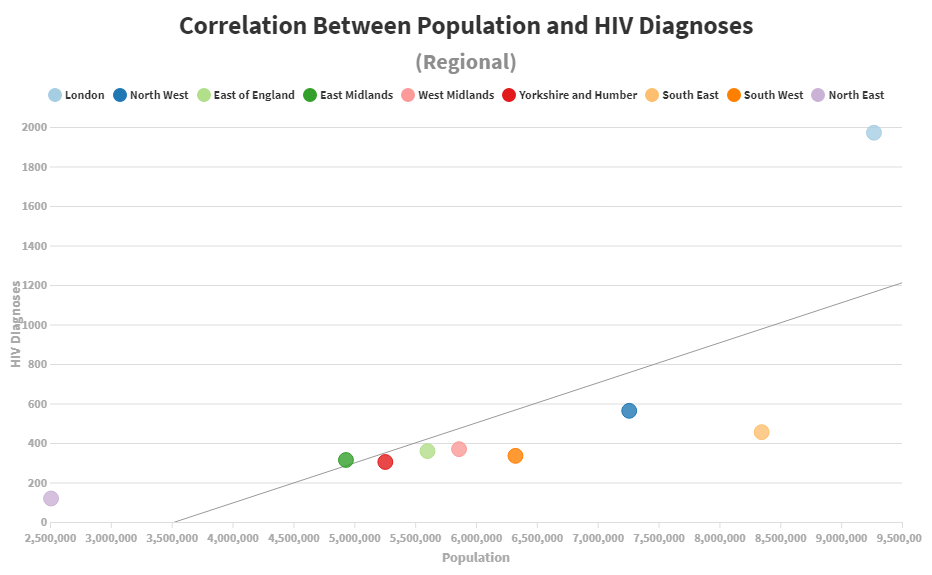
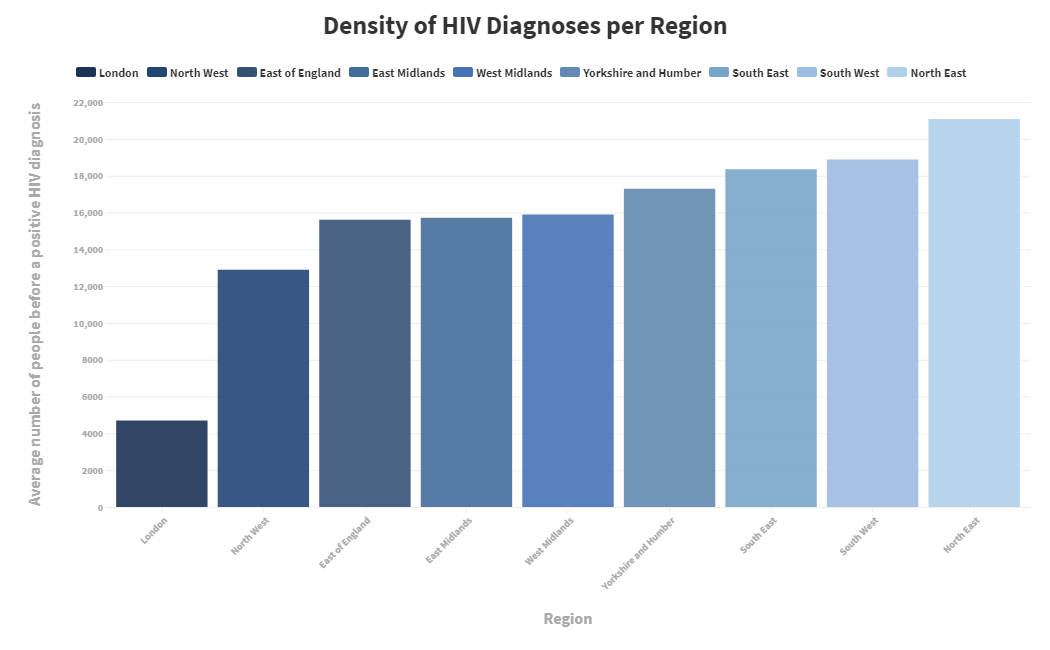
However, it's important to remember that there are more factors at play than just the amount of new diagnoses, so to understand the density of new HIV diagnoses per region in England, we divided the population of an area by the amount of new HIV diagnoses. With density in this situation, it's important to remember that the lower the number is, the higher the HIV rates are. For example, the population of the West Midlands is 5,860,700, and the number of new HIV diagnoses in 2017 was 369, meaning the density is 15,882. In other words, according to average statistics, every 1 in 15,882 people in the West Midlands was diagnosed with HIV in 2017. The graph shows London as having the highest density of new HIV diagnoses, with an average of 1 in every 4,703 people diagnosed with the virus in 2017.
We can also see that although London and the North East were still 1st & 9th respectively, most other regions changed places.
Looking at the figures per upper-tier local authority (UTLA), the regions with the highest instances of new HIV patients in 2017 included a range of towns and cities from across the country, but there was still a large portion of London areas. This ties in with the results that show that London has the highest amount of HIV diagnoses, as well as having the highest density. However, without looking at the population, the UTLA with the most diagnoses comes from the North West - Manchester.
The graph shows the 10 UTLAs with the highest number of HIV diagnoses in 2017 in descending order:
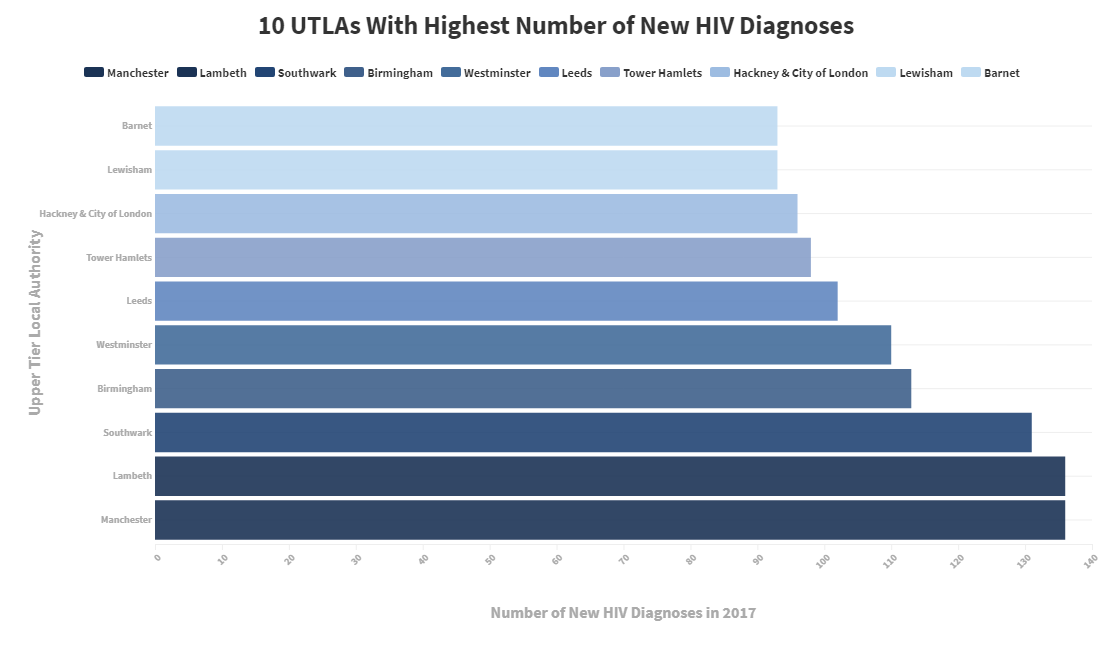
Manchester and Lambeth are the two UTLAs that have the highest amount of new HIV patients. As the mean number of diagnoses per UTLA is 32, all of these local authorities in the list sit well above the national average. Where Manchester is concerned, this is particularly interesting, as it's three times smaller than the UTLA of Kent, yet it has more than double the instances of HIV. But where do the above areas stand in terms of density? To work this out, we used the same formula as we did to work out regional density but applied it to each unique UTLA to find out whether the list changed at all.
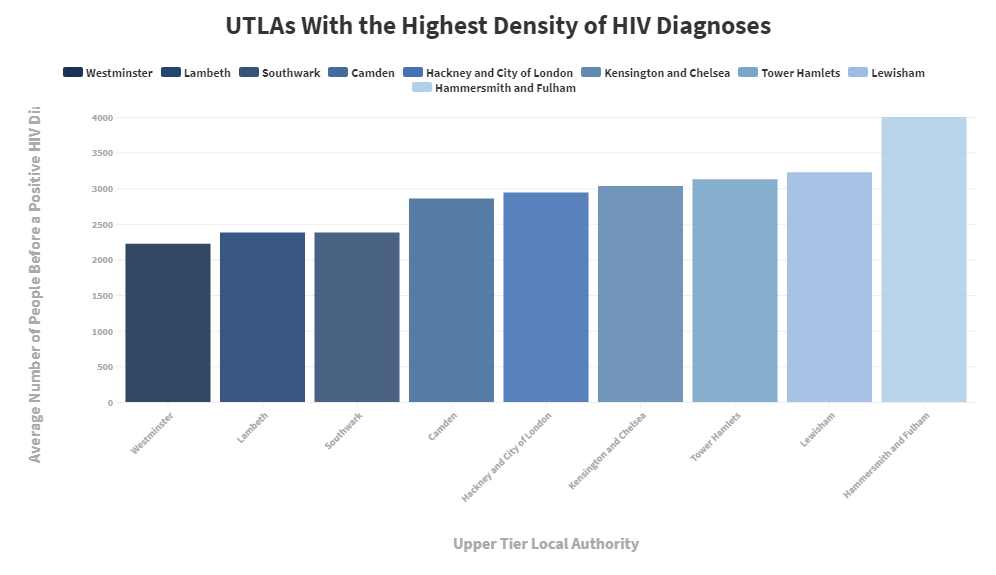
As you can see from the chart, Manchester, Leeds, and Birmingham have disappeared. This is because when the population is taken into account, some areas will have a higher density than others, so Manchester, Birmingham and Leeds are no longer on the list because the HIV diagnoses are more proportionate to the population than other UTLAs.
However, what's most interesting about this density chart is the fact that all of the listed UTLAs are in the London region, which shows that HIV prevalence in London Boroughs is higher than anywhere else in the country. Once again, this supports the results that state that regionally, London has the highest density of HIV diagnoses in relation to its population.
HIV Statistics London
From the results above, we already know that HIV prevalence in London boroughs is the highest of the entire country, but what is the reason for it?
The population of London (including Greater London) is almost at 10 million - the highest out of any other region in the country, especially when you consider its size in relation to regions such as the North West, so it's hardly surprising that HIV transmissions are higher in London than anywhere else in the UK. Due to the size of the area, we decided to look at HIV in London in more detail to see exactly where is most affected by new diagnoses. 
The chart shows us that Central and North London are the most affected areas in the region, whilst the outskirts and suburbs are generally less affected than those in the heart of the city. This would suggest that those living in central London are more at risk of HIV transmission and may need more support than those surrounding the capital. This can be done by allocating more IMPACT trial clinics within the centre and making it easier for people in need to access the drug.
Annual epidemiological spotlight on HIV 2017 - Links










